Contributing physicians in this story
Football and soccer players tend to be at risk for a concussion, however, the injury can happen to anyone. In fact, every 21 seconds, one person in the United States experiences a traumatic brain injury (TBI).¹ A TBI can be a serious head injury causing permanent disability or death; however, of the 1.5 million Americans who sustain a TBI each year, 75% of the injuries are concussions or other minor head injuries.²
Any blow or jolt to the head, some of which seem harmless, can cause a concussion. Falling off a ladder, falling in the bathtub, or tripping on a rug are just a few ways you can sustain a concussion in your home. A concussion can also occur while playing a contact sport such as baseball or football, while skating, or while riding a skateboard.
What is a concussion?
A concussion is not just a bump on the head or a rattling of the brain. It is a mild brain injury that results in a temporary change in brain function. The brain is composed of soft tissues encased within the hard bone of the skull. A concussion occurs when your head is hit or jolted and your brain’s soft tissue moves in reaction to the sudden force. At impact with the skull, the brain can become bruised, tissues can be torn, and minor swelling can occur (Fig. 1). An injury to the brain can cause neurons (nerve cells) and nerve tracts (neurological pathways) to change or not function properly. The changes in brain function can change the way you think, act, or feel.
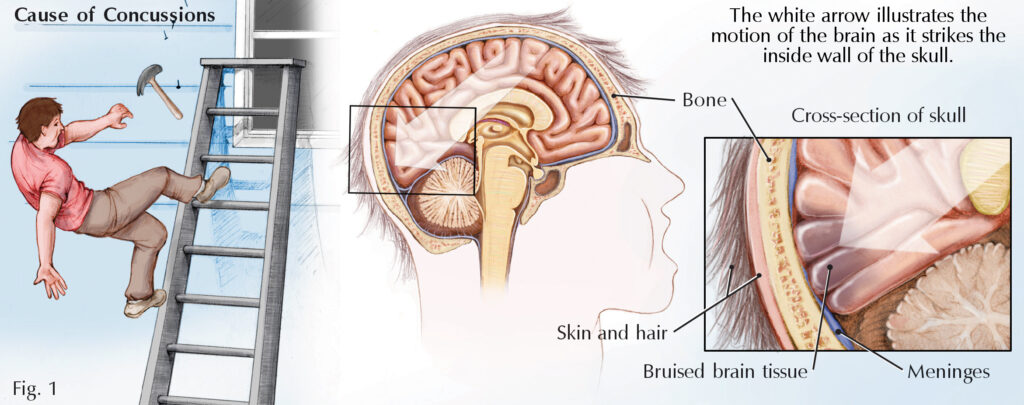
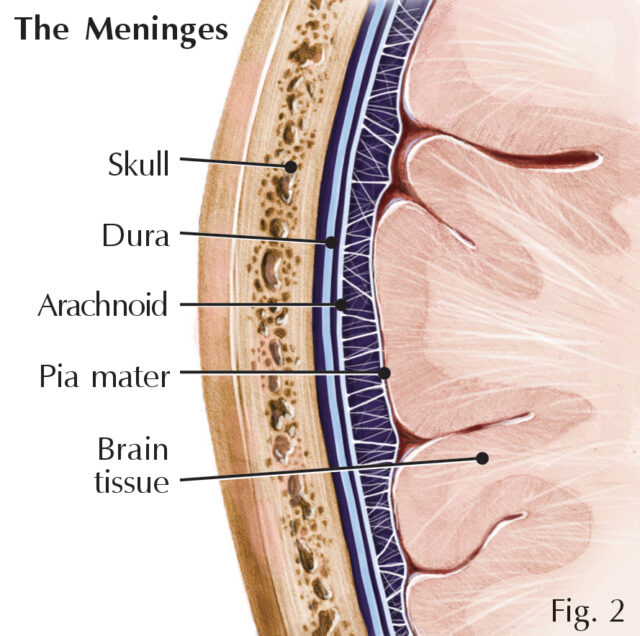
Three membranes, collectively called the meninges, provide protection by separating the brain’s soft tissue from the rigid wall of the skull. Three layers cover the brain; the dura, a tough, leathery outer covering; the arachnoid, a thin inner layer with threadlike strands that attach it to the pia mater; and the pia mater, which is a thin, delicate layer tightly attached to the surface of the brain (Fig. 2). In addition to the protection of the layers, cerebrospinal fluid surrounds the brain and cushions it as well. Even with these protections, the meninges and deeper tissues within the brain can become bruised when there is a blow or jolt to the head or when the head is severely jarred or shaken.
How do you know you have a concussion?
You cannot be absolutely sure you have a concussion until a physician examines you and a computerized axial tomography (CAT) scan or a magnetic resonance imaging (MRI), a scan that shows the bones, muscles, tendons, and ligaments, is completed and viewed. After a head injury, you should watch for signs and symptoms of a concussion and let your physician know what you have experienced. Your brain is as unique as you are and no two injuries are exactly alike; therefore, you can experience a variety of symptoms after a head injury. Some signs and symptoms of a concussion are a headache that does not go away easily or is more severe than normal, a stiff neck, nausea and vomiting, confusion that does not improve or gets worse, difficulty walking and using your arms, difficulty talking, and unusual sleepiness. Usually, you will not lose consciousness; however, loss of consciousness often means you sustained a more serious head injury.
Immediately after you injure your head, you may feel dizzy or confused and your head will probably hurt. A bruise or bump can appear very quickly and you may feel nauseated. Your vision may be blurred and you may not remember exactly what happened. If the symptoms of a concussion do not last very long, it does not mean you are uninjured. Some symptoms appear right away, while others do not show up for days or weeks after the injury.
Screening and diagnosis
To diagnose your injury, your doctor will examine the site of impact, and he or she will test your strength, balance, reflexes, sensation, and memory. The physician will ask you and anyone who witnessed the injury about how it occurred and about your behavior after the injury. A CAT or MRI scan will be taken to detect any bruising or swelling of the brain.
Treatment
A concussion heals with time and plenty of rest. For headaches, you can take acetaminophen, such as Tylenol™, but avoid aspirin, blood thinners, and any drug that causes drowsiness. Your doctor may assign a responsible family member or friend to wake you every few hours while you sleep to monitor any increase or change in your symptoms. Until all symptoms have subsided and your doctor has cleared you, you should avoid activities that might jolt your head again, such as playing a sport or riding an amusement park ride.
Second-Impact syndrome
Second-impact syndrome often occurs when an athlete returns to play too soon after a concussion. If an athlete has suffered a head injury, all signs and symptoms of a concussion should be resolved before he or she returns to play. Second-impact syndrome can cause permanent disability and death if a second injury occurs before the first has healed. Even a mild second injury can cause a loss of automatic control of blood vessels to the brain, causing severe swelling and damage to brain tissues.
If your first head injury is mild, you can sometimes return to your sport during the game; however, depending upon the severity of your injury and the symptoms, you may not return to the sport for days or weeks. After numerous head injuries, your physician may recommend that you find another sport. Second impact syndrome can occur when anyone, not just athletes, sustains a second or third concussion before the previous head injury has healed. Therefore, it is important that you receive clearance from your doctor before you return to any activity that can put you at risk for another head injury.
You are at a higher risk for a concussion to occur if you play a contact sport; however, more concussions occur off the field than on each year. Falls in your home and automobile accidents top the list of causes of head injuries. To avoid a concussion, do what you can to protect yourself; wear a seatbelt and wear a helmet when riding a bike, motorcycle, horse, or skateboard. Make your home as fall-proof as possible by removing area rugs that slide, installing handrails, and using non-slip mats in the bathtub and shower.
For more information about brain injuries and how to prevent them, visit the Brain Injury Association of America’s Web site at www.biausa.org and the Centers for Disease Control and Prevention’s (CDC) Website at www.cdc.com.
Author: Patrick J. Fernicola, MD | Columbus, Georgia
References:
1. Brain Injury Association of America. www.biausa.org/Pages/what_is_brain_injury.html. Accessed 5/3/05.
2. Centers for Disease Control and Prevention. www.cdc.gov/. Traumatic Brain Injury-Fact Sheet. Accessed 5/3/05.
Last edited on October 15, 2021