Contributing physicians in this story

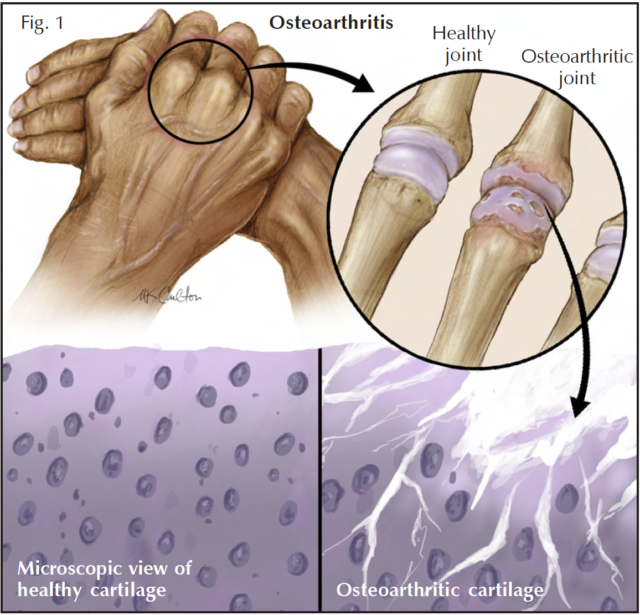 Affecting 21 million Americans, osteoarthritis is one of the most common forms of arthritis in the United States. Arthritis and related conditions such as osteoarthritis cost the US economy nearly 86 billion dollars per year in medical care and indirect expenses, including lost wages and production.1 Thus, osteoarthritis is a serious US health concern, with great economic impact.
Affecting 21 million Americans, osteoarthritis is one of the most common forms of arthritis in the United States. Arthritis and related conditions such as osteoarthritis cost the US economy nearly 86 billion dollars per year in medical care and indirect expenses, including lost wages and production.1 Thus, osteoarthritis is a serious US health concern, with great economic impact.
The good news is osteoarthritis can often be effectively treated using treatment modalities, including rest, activity modification, anti-inflammatory medications, injections of medication, braces, and canes. When these treatments are no longer effective, a variety of surgical approaches may be considered, including arthroscopic surgery (only in specific instances), limb realignment surgery, and joint replacement surgery.
Increasingly, patients are educating themselves about their disease. And while heightened patient awareness almost always leads to better patient decision making, misinformation can have the opposite effect.
So what are the myths, and what are the current realities about osteoarthritis and its treatment?
Myth 1: Osteoarthritis is “wear and tear” arthritis.
The truth is we do not know the exact cause of osteoarthritis. But we do know it is more than just mechanical wear and tear. Mechanical, biochemical, and genetic factors probably all play a role in the disease (Fig. 1). In addition to mechanical forces, cartilage is destroyed in osteoarthritis by powerful enzymes called metalloproteinases. These substances slowly destroy the interior framework of cartilage. The role of genetics in osteoarthritis is still being defined. Osteoarthritis has been known to run in families, and occurs routinely in certain patients with known genetic defects of cartilage.
Myth 2: Osteoarthritis is potentially reversible.
There is little scientific evidence of treatment approaches for osteoarthritis that halt the progression of the disease. And there is no scientific evidence that the disease process can be reversed. Limiting excessive impact loading of the joints may slow disease progression, and reduce pain. Therefore, weight control and exercise is an important factor in slowing the progression of the disease.
Myth 3: Cartilage “protective” agents: The truth about glucosamine and chondroitin sulfate.
Glucosamine and chondroitin sulfate are nutritional supplements available over-thecounter. Many patients believe these agents halt the progression of arthritis, or can cause cartilage to grow back in their joints. Current scientific evidence suggests that these agents are only effective in alleviating arthritic pain. Evidence that they change the course of arthritis is scant and questionable. I recommend trying the medications for 4 to 6 weeks, and then continuing them only if they are relieving pain.
Myth 4: Non-steroidal anti-inflammatory medications (NSAIDS) are dangerous and should be avoided.
The potential dangers of NSAIDS have received a great deal of media attention recently. Specifically, some reports have shown an increased risk of heart attacks with some of these medications. Two medications have been taken off the market (Vioxx and Bextra). Celebrex was linked to heart attacks only in patients who already had heart disease and who were taking very high doses of the medication. The FDA has concluded that NSAIDS are generally safe at prescription strength doses but should be used with caution in patients with heart disease. Remember, all medications can have serious side effects, especially if patients take more than the prescribed dose. And patients taking NSAIDS for more than 6 months need periodic blood tests for liver and kidney function. NSAIDS continue to play a vital role in the day-to-day treatment of arthritis. Increased awareness about the potential side effects of these medications will help patients use them wisely.
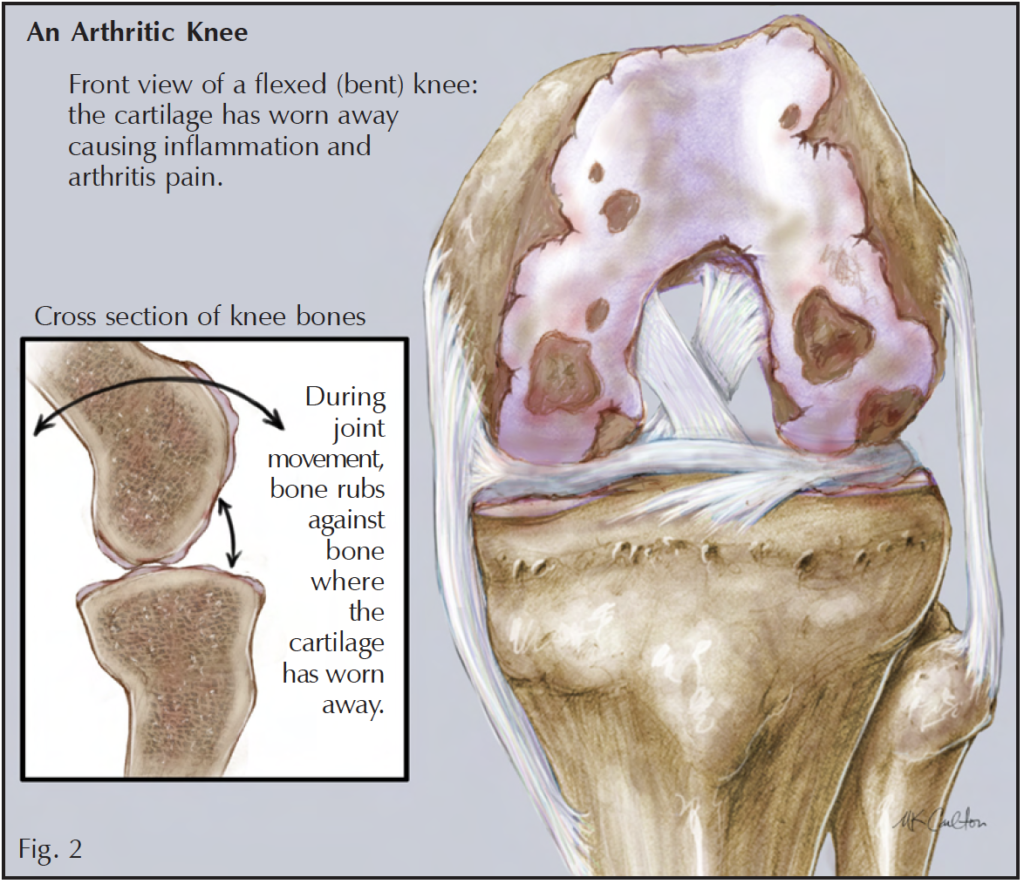
Myth 5: Cortisone shots just mask the pain and are therefore worthless.
Cortisone shots are hardly worthless. Because there is no known cure for arthritis, the goal is to alleviate symptoms and prolong joint replacement surgery. Arthritis pain comes from 2 principle sources: the irregular joint surfaces that rub together, and inflammation (Fig. 2). Cortisone relieves pain by reducing the level of inflammation. Injections may be safely administered every 3 to 4 months, with no more than 10 to 15 injections in any single joint over one’s lifetime.
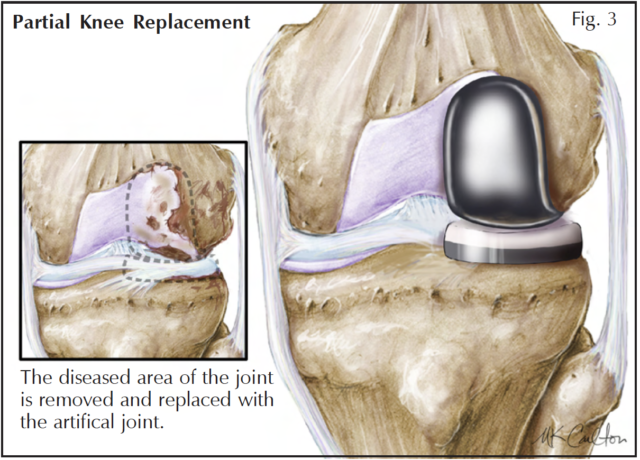
Myth 6: Total joint replacement is the only option for patients with severe arthritis.
Again, this depends on the specific situation. Patients with arthritis affecting only one side of the knee are potential candidates for less invasive operations. Young patients desiring to be physically active can consider a realignment osteotomy of their knee, which changes the weight-bearing axis of the leg, and transfers much of the forces of weight bearing away from diseased cartilage. Partial knee replacement involves replacing only that portion of the joint that is diseased, leaving the unaffected portion intact (Fig. 3). Using modern instruments, this procedure can now be performed through a small incision with a much shorter hospital stay of 1 to 2 days. The cure for arthritis has proven to be as elusive as the cure for cancer, but medical researchers are hard at work searching for solutions. New directions for treatment include the use of cartilage cells to reconstitute damaged cartilage, and gene therapy. In the mean time, treating the symptoms of arthritis using a well-reasoned, balanced approach continues to be our best treatment option.
Author: James E. McGrory, MD | Columbus, Georgia
References:
1. Osteoarthritis Fact Sheet. Arthritis Foundation. www.arthritis.org/conditions/Fact_Sheets/OA_Fact_Sheet.asp. Accessed July 31, 2006.
Last edited on October 18, 2021